What is a Spinal Cord Injury/Disorder
What is a Spinal Cord Injury?
Spinal cord injury (SCI) refers to any damage to the spinal cord, whether from trauma, disease, or a degenerative disorder. This may result in loss of movement, sensation and changes in autonomic functions such as blood pressure and temperature control.
The spinal cord is a bundle of nerves that transmits messages between the brain and the rest of the body. The spinal cord runs from the base of the brain through the center of the vertebrae and is protected by the spinal column.
The Spine and Spinal Cord
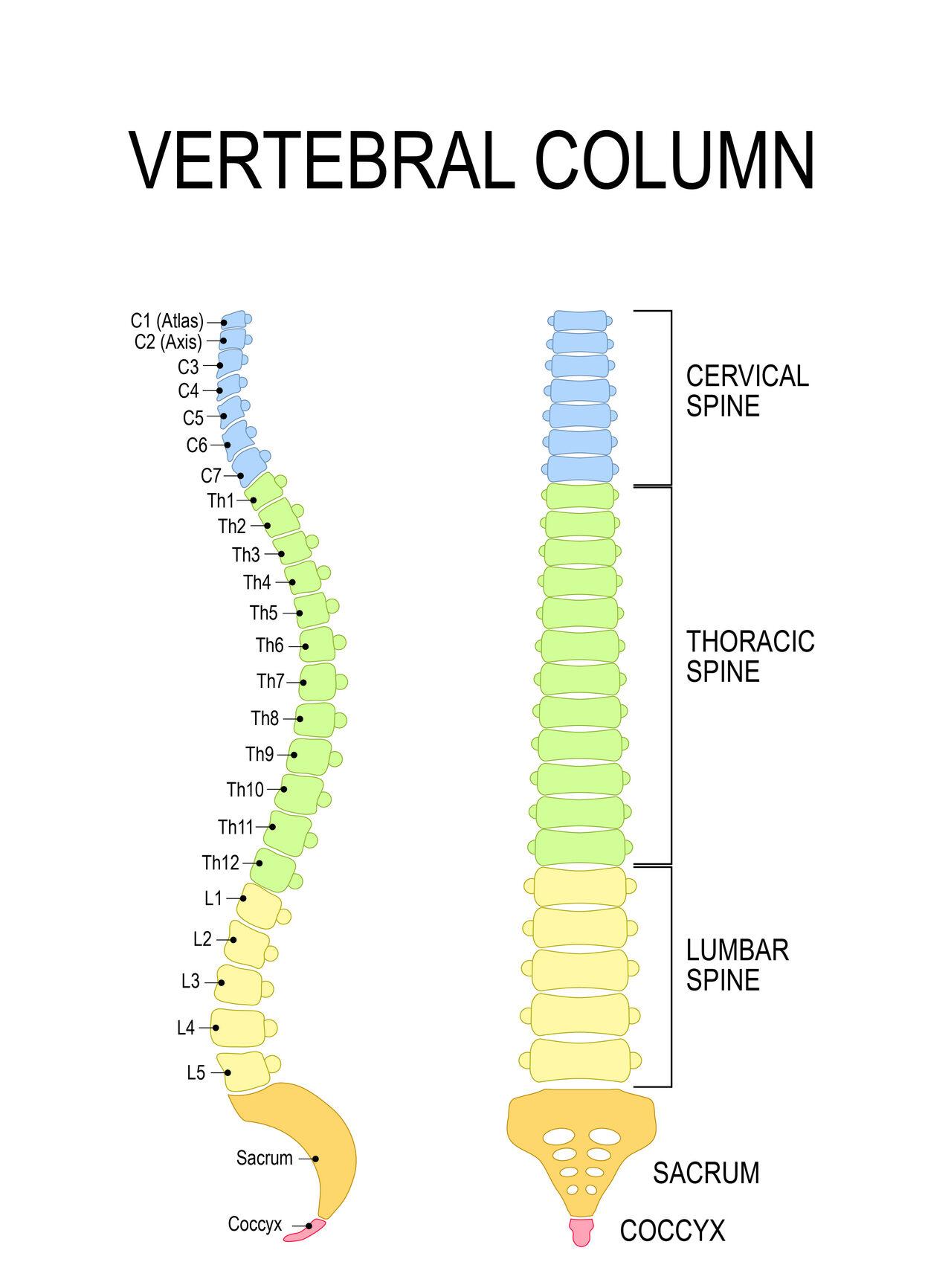
The spine consists of 33 bones, known as vertebrae. There are seven cervical (neck region), 12 thoracic (upper and mid back), five lumbar (lower back), five sacral (fused together as part of the pelvis), and 3-5 coccygeal (fused as the “tailbone”) vertebrae.
The spinal cord is divided into 31 segments, from which the spinal nerves emerge on each side of the body, between adjacent vertebrae. The spinal nerves extend to various parts of the body, delivering messages from the brain to the body and from the body to the brain. There are eight cervical segments, 12 thoracic segments, five lumbar segments, five sacral segments and one coccygeal segment. The spinal cord is shorter than the spine, and while there are some anatomical differences among individuals, the spinal cord ends roughly near the first lumbar vertebra.

After a spinal cord injury, nerves above the level of injury keep working as they did before. But below the level of injury, messages from the brain to the body and messages from the body to the brain may become fully or partially blocked due to traumatic injury, degenerative conditions, or disease. Reflexes are also impacted.
Depending on the extent of the injury, the higher the level at which spinal cord damage occurs, the greater the degree of impairment. For example, injuries to the upper cervical (neck) region may result in paralysis (lack of movement) of the arms, hands, legs, feet, and respiratory muscles, as well as impaired bowel, bladder, and sexual function. Spinal cord injury that results in some degree of paralysis in all extremities is referred to as tetraplegia (also known as quadriplegia).
In contrast, people with thoracic and lower injuries may experience paraplegia, retaining full use of their arms and hands, but experience some paralysis in the legs. These injuries may also result in bowel, bladder and sexual function changes.
For more information on the spinal cord, see the Model Systems of Knowledge Translation Center’s factsheet, Understanding SCI Part I: The Body Before & After Injury.
Spinal Cord Injury Statistics
According to the National Spinal Cord Injury Statistical Center, every year, approximately 18,000 Americans acquire a traumatic spinal cord injury. The Statistical Center has collected data on patients with traumatic SCI treated at the Spinal Cord Injury Model Systems since the 1970s.
Of those included in the database, roughly 79% are men, and the average age at injury is 43. Most traumatic spinal cord injuries happen because of a vehicle accident (37.6%), followed closely by falls (31.5%), trailed by violence (15.4%), sports (8.3%), and medical/surgical causes (3.6%)
For more data related to traumatic spinal cord injury, please see “Traumatic Spinal Cord Facts & Figures at a Glance,” a publication by the National Spinal Cord Injury Statistical Center.
Spinal Cord Injury Symptoms and Signs
The symptoms of a spinal cord injury can vary widely depending on the location and severity of the injury. Common signs and symptoms of a spinal cord injury may include paralysis (inability to move muscles or muscle weakness below the level of injury, loss of sensation or changes in sensation, altered reflexes and changes in autonomic functions such as sweating and blood pressure control. Other symptoms include pain, loss of bowel and bladder control, and difficulty breathing.
Spinal Cord Injury Levels
The neurological level of injury refers to the lowest level of the body where sensation and movement are intact. The level of the injury helps describe the extent of functional impairment. It is determined by an examination that evaluates muscle strength in key muscle groups, tests sensation to pinprick and light touch throughout the body and assesses the ability to contract the anus voluntarily and the presence of anal sensation. This exam is known as the International Standards for Neurological Classification of Spinal Cord injury (ISNCSCI) sometimes referred to as the American Spinal Injury Association (ASIA) Exam.
Incomplete and Complete Spinal Cord Injury
Understanding the neurological level and completeness of an SCI is essential for medical diagnosis, treatment planning, and determining the functional goals for rehabilitation and maximizing recovery. Spinal cord injuries are often referred to as either an incomplete or complete injury.
What is an incomplete spinal cord injury?
An incomplete spinal cord injury means there is some preserved neurological function at the lowest part of the spinal cord, which is exhibited by the ability to voluntarily tighten the anus and/or some feeling in the anal area. Incomplete spinal cord injuries occur when the spinal cord is partially damaged. They can vary in severity, and the degree of impairment can range from mild to severe.
Common characteristics of incomplete spinal cord injuries include partial loss of motor function or partial loss of sensation below the injury level. Some individuals may experience significant motor and sensory function improvement over time, while others with similar levels of injury may not.
Spinal cord injury neurological levels are typically described using a combination of letters and numbers (for example, C5 B). The first letter refers to the region of the spinal cord involved (cervical in this example), and the number refers to the specific segment within the spinal region (the fifth cervical segment in this example). The higher the number, the further down the spine the injury occurs within that spinal region. The final letter indicates the severity of impairment reflected by the ASIA Impairment Scale (AIS), which describes the extent of impairment.
A sensory incomplete injury, referred to as AIS B, indicates that some sensation is intact below the level of injury at the anal area, but no, or limited, motor function is noted below the injury. A motor incomplete injury classified as AIS C indicates that there is voluntary anal contraction or sensation in the anal area and weak motor function below the level of the injury (more than half of the key muscles below the level of injury cannot move against gravity). A motor incomplete injury classified as AIS D is similar to AIS C, except half or more of the key muscles below the level of injury can move against gravity.
Two people with seemingly similar incomplete injuries may have very different outcomes and levels of impairment based on the unique characteristics of their injuries. The effectiveness of their treatment and rehabilitation can also impact their functional outcomes.
What is a complete Spinal Cord Injury?
A complete spinal cord injury occurs when the spinal cord is damaged to the extent that there is no sensation in the anal area and no voluntary ability to tighten the anus. This is graded as AIS A. Some individuals with complete injuries may retain some minimal movement and sensation below the level of injury (but not in the anal area), and this is known as the zone of partial preservation. A complete spinal cord injury does not necessarily mean that the cord is completely severed (a common misconception). It is possible to have a complete injury initially that over time improves to an incomplete injury.
Other features of a complete spinal cord injury may include impaired autonomic function. Control over blood pressure, heart rate, body temperature, and bowel/bladder control may become compromised. While this is also true of incomplete injuries, the impacts may be less severe in incomplete cases of SCI.
Functional Capabilities:
Cervical Region (C1 to C8): Injuries in the cervical region are injuries to the highest part of the spine and may be the most disabling. They affect the neck and upper spine, legs, trunk, respiratory muscles, bowel and bladder. Changes in autonomic functions such as blood pressure and temperature control, heart rate, and sweating are also impacted.
Thoracic Region (T1 to T12): Injuries in the thoracic region occur in the back. Thoracic injuries often result in paraplegia (paralysis of the lower body and legs) but full function of arms and hands is expected. Abdominal muscles and chest muscles may be affected and impact balance and trunk control at higher thoracic levels, but those with lower thoracic injury will generally have improved balance due to the sparing of chest and abdominal muscles. Bowel, bladder, and sexual function are also often affected.
Lumbar Region (L1 to L5): Injuries in the lumbar region affect the lower back and the lower limbs. Complete Lumbar injuries typically result in paraplegia, with varying degrees of impairment in the legs and impairments of bowel, bladder, and sexual function.
Sacral Region (S1 to S5): The sacral vertebrae are fused. Sacral region injuries are the lowest, affecting the pelvis. Injuries in this region may affect bowel, bladder, and sexual function. Injuries in this region still allow for some control of the legs and feet.
For more information on injury levels and functional goals, see the Functional Goals Chart on this Model Systems Knowledge Translation Center Factsheet.
Spinal Cord Injury Treatment
The treatment of a spinal cord injury typically involves emergency medical care, surgical intervention in many cases, and ongoing rehabilitation and management. The specific approach to treatment may vary depending on the type and severity of the injury.
Directly following the injury, immediate assessment and stabilization are crucial. This includes maintaining the airway, ensuring breathing and circulation, and immobilizing the spine to prevent further damage.
Inpatient rehabilitation is a critical part of SCI treatment. Inpatient rehabilitation aims to help people learn about their condition and how to manage their health moving forward and regain as much function and independence as possible. Inpatient rehabilitation typically involves a multidisciplinary rehabilitation team that may include physiatrists (doctors of physical medicine and rehabilitation), nurses, social workers, psychologists and physical, occupational, speech, and respiratory therapists.
Assistive devices like wheelchairs, braces, and adaptive equipment to enhance mobility and independence may be recommended. Once the individual has stabilized and achieved their inpatient rehabilitation goals, they may proceed with outpatient rehabilitation therapies to maximize their functional independence.
Medications may be prescribed to manage various aspects of SCI, including pain, muscle spasticity, bladder and bowel management issues. and complications like urinary tract infections.
Assistive technologies and adaptive devices can greatly improve the quality of life for individuals with SCI. These may include customized wheelchairs, voice-activated devices, smart home technologies, and other assistive technology.
The exact treatment plan for spinal cord injury should be individualized based on the patient’s specific condition, level of injury, and personal goals. It is important for individuals with SCI to work closely with a multidisciplinary team of healthcare professionals, to ensure comprehensive and effective care.
Spinal Cord Injury Complications
Because SCI impacts many bodily functions, there are some secondary health complications that can occur. It’s important for individuals with SCI to learn about their condition and the best methods for preventing possible complications. This teaching is often initiated during inpatient rehabilitation.
Reduced weight-bearing and lack of mobility can lead to bone loss (osteoporosis) and an increased risk of fractures. Prolonged immobility can lead to contractures, which can lead to permanent joint deformities restricting movement.
Immobility, poor sensation, and incontinence can also lead to the development of pressure injuries (bedsores). Pressure injuries are a serious complication of SCI and develop when there is too much pressure impacting blood flow, which can damage skin and underlying tissues. Education programs are focused on learning to prevent pressure injuries through pressure relieving techniques and appropriate equipment, learning to identify risks and signs of pressure injuries, and how to manage them if they develop.
Some individuals may develop heterotopic ossification, or abnormal bone growth in soft tissues, limited joint mobility and pain in some cases. Also, reduced mobility and changes in blood flow can increase the risk of deep vein thrombosis (DVT), commonly referred to as blood clots, which can potentially travel to the lungs, causing a pulmonary embolism (PE).
Spinal Cord Injury’s Impact on Bowel and Bladder Function
Changes in bowel and bladder function can lead to additional complications such as constipation, incontinence, and urinary tract infections. SCI typically impacts an individual’s ability to voluntarily empty their bowels and bladder.
Bladder management strategies such as intermittent catheterization or indwelling catheterization can help with bladder emptying to minimize complications such as urinary tract infections. Bladder management methods are individualized based on the level of injury, bladder function, hand function, availability of assistance and more. Physicians with spinal cord injury expertise can help find the best bladder emptying option together with the individual.
Bowel management programs are established to promote routine bowel emptying, prevent constipation, and minimize bowel accidents. Bowel management programs aim to promote routine bowel emptying using various methods such as timing, diet, medications, and bowel management techniques such as digital stimulation or digital removal.
Autonomic and Other Cardiovascular Complications
Autonomic functions such as heart rate and blood pressure control may be affected. Autonomic dysreflexia is a serious complication that can occur in individuals with neurological levels at T6 or above. This is considered a medical emergency when it occurs.
Autonomic dysreflexia occurs when irritating stimuli below the level of injury sends signals that cause blood vessels to constrict. Because of the spinal cord injury, messages that normally would be sent to relax the blood vessels are impaired. This can cause a dramatic increase in blood pressure which can lead to serious complications.
Symptoms of autonomic dysreflexia include increased blood pressure, pounding headache, sweating, changes in heart rate, nasal congestion, blurred vision and more. Treatment involves steps to lower the blood pressure and identifying and eliminating the source of irritation. Emergency medical intervention may be required.
Other cardiovascular complications that may occur include orthostatic hypotension, meaning low blood pressure when moving from lying to sitting or standing positions, resulting in dizziness or fainting in some cases. Nonpharmacological approaches, such as the use of an abdominal binder or compression stockings, can help, and medication management may be needed in more severe cases.
Additional Complications to Monitor
Spasticity can be a troublesome complication following SCI. Spasticity may exhibit as increased tone in muscle, involuntary muscle movements, and increased exaggerated reflex responses. While some degree of spasticity can help maintain muscle tone, more severe spasticity can interfere with activities of daily living and, in some cases, become a safety concern.
There are multiple treatment options available, including nonpharmacological approaches. Medications include oral medications, botulinum toxin injections, and intrathecal baclofen therapy, which requires a surgical procedure.
Spinal cord injury often results in significant lifestyle changes, including the need for caregiving support and adaptive equipment. This can lead to role changes and financial and social challenges. The consequences of SCI can result in depression, anxiety, and other psychological challenges. Fortunately, help is available via peer support and mental health providers.
How a Spinal Cord Injury Affects the Brain
Some people wonder if a spinal cord injury will have some impact on cognition (thinking and memory). The most direct effect of an SCI is the impairment of sensory, motor, and autonomic function below the level of the injury and does not affect cognition.
Some individuals, particularly those who have upper neck injuries, may also sustain a brain injury at the time of injury. This is known as a traumatic brain injury (TBI). The effects of TBIs may range from mild to severe. To learn more about TBI, please read this factsheet by the Model Systems Knowledge Translation Center.
Signs of recovery from a spinal cord injury
Naturally, people with SCI want to know their prognosis for recovery. There is currently no proven method to restore function following a spinal cord injury completely, and it’s not possible to guarantee if or how much improvement an individual might experience. In this section, the word recovery refers to overall improvements in health and function rather than a complete restoration of function.
Recovery from a spinal cord injury varies widely among individuals and depends on various factors, including the level and severity of the injury, the type of treatment and rehabilitation received, and the individual’s overall health. While it’s not possible to guarantee how much improvement a person will make, many people make some degree of improvement following SCI. Areas for potential improvement include:
- Improved severity of injury, for example, some individuals gain muscle strength and moving from an AIS C to D or regain some sensation in areas previously affected by numbness or loss of feeling.
- Some people with complete SCI regain one or two levels of function, meaning they regain some mobility in one or two muscle groups below their level of injury which can lead to increased overall capabilities.
- Improvement in functional abilities often occurs, such as learning new skills, using adaptive equipment to complete activities, and improving strength in weak muscles and muscles unaffected by SCI.
People with incomplete injuries are generally more likely to regain some muscle movement than people with complete injuries. Also, your chances for more movement are better the more gains that you see. Achieving rehabilitation goals and meeting milestones is encouraging.
Every Spinal Cord Injury is Unique
It is important to note that recovery from an SCI can be a slow and ongoing process, and the extent of recovery varies widely among individuals. In some cases, recovery may be limited, while in others, significant gains in function may be possible. Early and intensive rehabilitation and a comprehensive treatment plan can improve the chances of overall improvements in health. Patients work together with their healthcare team to set achievable goals and monitor progress throughout the rehabilitation process.
Each spinal cord injury is unique, and improvement will depend on the individual circumstances. Patience, persistence, and a positive attitude are important throughout the recovery journey.
United Spinal Association proudly partners with the Model System Knowledge Translation Center, which provided many of the resources in this article. Contact United Spinal Association’s Community Support team for more information or assistance. Join our community by signing up for a free membership. To support our mission, donate here.
